DIABETIC NEEDS AND EQUIPTMENT
The typical Blood Glucose monitors we carry are several.
One touch
Contour
Accu Check
True Metrix
Embrace
Freestyle
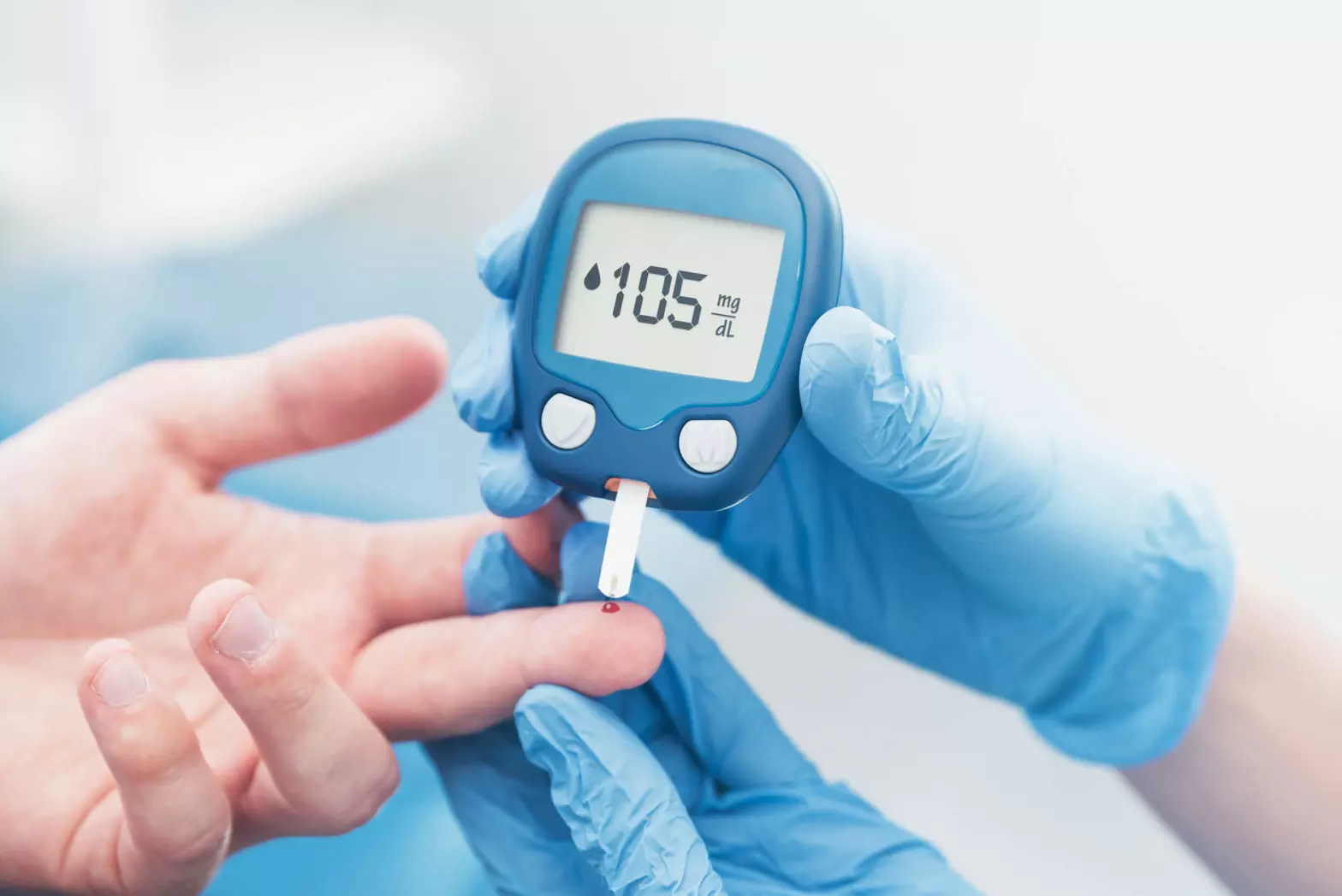
Regular blood sugar monitoring is the most important thing you can do to manage your diabetes. You’ll be able to see what makes your numbers go up or down, such as eating different foods, taking your medicine, or being physically active. Armed with this information, you can better work with your health care team to make decisions about your best diabetes care plan. These decisions can help delay or prevent diabetes complications such as heart attack, stroke, kidney disease, blindness, and amputation. Your doctor will tell you when and how often to check your blood sugar levels.
Most blood sugar meters allow you to save your results and you can use an app on your cell phone to track your levels. If you don’t have a smart phone, keep a written daily record. You should bring your record with you each time you visit your health care provider.
HOW TO USE A BLOOD SUGAR MONITOR
Make sure the meter is clean and ready to use.
After removing a test strip, immediately close the test strip container provided tightly. Test strips can be damaged if they are exposed to moisture, extreme heat, or cold temperatures.
Wash your hands with soap and warm water. Dry well. Massage your hand to get blood into your finger. Use a lancet to prick your finger. Squeezing from the base of the finger, gently place a small amount of blood onto the test strip. Place the strip in the meter.
After a few seconds, the reading will appear. Track and record your results. Properly dispose the lancet and strip in a trash container.
Do not share blood sugar monitoring equipment, such as lancets, with anyone, even other family members. In addition to you, have someone else learn how to use your meter in case you’re sick and can’t check your blood sugar yourself.
CONTINUOUS BLOOD GLUCOSE MONITORS
Glucose meters are a great tool, but sometimes you need to keep a closer eye on your blood sugar levels. That's where a device called a continuous glucose monitor can help. This FDA-approved system tracks your blood sugar automatically throughout the day and night. It collects readings every 5 to 15 minutes. You can see your blood sugar level anytime. Here at Union Prescription Center and Medical Supplies we carry Freestyle Libre and Dexcom continuous glucose monitoring devices. Seeing glucose levels in real time can help you make more informed decisions throughout the day about how to balance your food, physical activity, and medicines. It can help detect trends and patterns that give you and your doctor a more complete picture of your diabetes. The data can help you find ways to better manage your condition. You need a prescription from your doctor to get one.
A CGM (continuous glucose monitoring device) works through a tiny sensor inserted under your skin, usually on your belly or arm. The sensor measures your interstitial glucose level, which is the glucose found in the fluid between the cells. The sensor tests glucose every few minutes. A transmitter wirelessly sends the information to a monitor.
QUESTIONS TO ASK YOUR DOCTOR
When visiting your doctor, you might keep these questions in mind to ask during your appointment.
1. What is my target blood sugar range?
2 .How often should I check my blood sugar?
3. What do these numbers mean?
4 .Are there patterns that show I need to change my diabetes treatment?
5. What changes need to be made to my diabetes care plan?
DIABETES MEAL PLANNING
A meal plan is your guide for when, what, and how much to eat to get the nutrition you need while keeping your blood sugar levels in your target range. A good meal plan will consider your goals, tastes, and lifestyle, as well as any medicines you’re taking.
A good meal plan should:
1. Include more non-starchy vegetables, such as broccoli, spinach, and green beans.
2. Have less added sugars and refined grains, like white bread, rice, and pasta that has less than 2 grams of fiber per serving.
3. Focus on whole foods NOT highly processed food.
Carbohydrates in the food you eat raise your blood sugar levels. How fast carbs raise your blood sugar depends on what the food is and what you eat with it. For example, drinking fruit juice raises blood sugar faster than eating whole fruit. Eating carbs with foods that have protein, fat, or fiber slows down how quickly your blood sugar rises.
You’ll want to plan for regular, balanced meals to avoid high or low blood sugar levels. Eating about the same amount of carbs at each meal can be helpful. Counting carbs and using the plate method are tools that can make planning meals easier.
COUNTING CARBS
Keeping track of how many carbs you eat and setting a limit for each meal can help keep your blood sugar levels in your target range. Your doctor or a registered dietitian can help you find out how many carbs you can eat each day and at each meal.
THE PLATE METHOD
It’s easy to eat more food than you need without realizing it. The plate method is a simple, visual way to make sure you get enough non-starchy vegetables and lean protein while limiting the amount of higher-carb foods you eat that have the highest impact on your blood sugar.
Start with a 9-inch dinner plate:
Fill half with non-starchy vegetables, like salad, green beans, broccoli, cauliflower, cabbage, and carrots. Fill one quarter with a lean protein, like chicken, turkey, beans, tofu or eggs. Fill one quarter with carb foods. Foods like grains, starchy vegetables, rice, pasta, beans, fruit, and yogurt. A cup of milk also counts as a carb food.
Then choose water or a low-calorie drink such as unsweetened iced tea to go with your meal.

